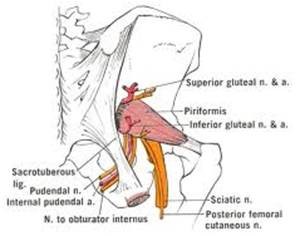
 The pudendal nerve is a somatic nerve within the pelvis comprised of branches of the sacral plexus levels S2-4. The pudendal nerve innervates the external genitalia in men and women including the labia, scrotum, penis, clitoris, and anus and provides motor function for bowel, bladder, and orgasm function. The pudendal nerve has three branches: perineal nerve, inferior rectal, and dorsal penile/clitoral. The pudendal nerve of the pelvis can become compressed (or entrapped) as it passes through the inside portion of the ischium or “sits bones” portion of the pelvis. The nerve path exits from the greater sciatic foramen, travels around the ischial spine, and passes through the lesser sciatic foramen. The pudendal nerve transverses through many other pelvic structures. It passes between the sacrotuberous and sacrospinous ligaments, between the piriformis and coccygeus muscles, and accompanies the pudendal artery and vein through the obturator fascia or Alcock’s (pudendal) canal. Compression or entrapment can occur at any of these sites along its path. A common cause of pudendal nerve entrapment is prolonged cycling on an incorrectly positioned or improperly shaped bicycle seat. This results in tension or thickening of the sacrotuberous and sacrospinous ligaments causing pudendal nerve entrapment between the ligaments. Other causes of pudendal nerve entrapment include pregnancy, pelvic floor muscle dysfunction, scarring due to pelvic surgeries, falls, sports injuries, horseback riding, and motor vehicle accidents. Chronic pain from pudendal entrapment can be felt in the abdomen, perineum, ischial tuberosities, buttock, vulva, clitoris, penis, scrotum, testicles, bladder/urethra, and anus. Most patients have increased pain upon sitting and have relief of pain upon standing, lying down, or sitting on a toilet seat. Symptoms can be pain, burning, numbness, and/or tingling in the pelvis and can radiate elsewhere. The pain is usually one-sided but there have also been cases where both sides are involved. Other symptoms may include urinary or fecal incontinence. An MRN can help with medical diagnosis.
The pudendal nerve is a somatic nerve within the pelvis comprised of branches of the sacral plexus levels S2-4. The pudendal nerve innervates the external genitalia in men and women including the labia, scrotum, penis, clitoris, and anus and provides motor function for bowel, bladder, and orgasm function. The pudendal nerve has three branches: perineal nerve, inferior rectal, and dorsal penile/clitoral. The pudendal nerve of the pelvis can become compressed (or entrapped) as it passes through the inside portion of the ischium or “sits bones” portion of the pelvis. The nerve path exits from the greater sciatic foramen, travels around the ischial spine, and passes through the lesser sciatic foramen. The pudendal nerve transverses through many other pelvic structures. It passes between the sacrotuberous and sacrospinous ligaments, between the piriformis and coccygeus muscles, and accompanies the pudendal artery and vein through the obturator fascia or Alcock’s (pudendal) canal. Compression or entrapment can occur at any of these sites along its path. A common cause of pudendal nerve entrapment is prolonged cycling on an incorrectly positioned or improperly shaped bicycle seat. This results in tension or thickening of the sacrotuberous and sacrospinous ligaments causing pudendal nerve entrapment between the ligaments. Other causes of pudendal nerve entrapment include pregnancy, pelvic floor muscle dysfunction, scarring due to pelvic surgeries, falls, sports injuries, horseback riding, and motor vehicle accidents. Chronic pain from pudendal entrapment can be felt in the abdomen, perineum, ischial tuberosities, buttock, vulva, clitoris, penis, scrotum, testicles, bladder/urethra, and anus. Most patients have increased pain upon sitting and have relief of pain upon standing, lying down, or sitting on a toilet seat. Symptoms can be pain, burning, numbness, and/or tingling in the pelvis and can radiate elsewhere. The pain is usually one-sided but there have also been cases where both sides are involved. Other symptoms may include urinary or fecal incontinence. An MRN can help with medical diagnosis.
How can Pamela Morrison Physical Therapy, P.C. help with PNE?
After a comprehensive evaluation with your pelvic expert, your diagnosis can be confirmed. Our physical therapists perform specific connective tissue techniques, such as skin rolling and myofascial release, around the nerve to release the compression or entrapment. Soft tissue mobilization and deep tissue massage may prove beneficial in relieving compression off of the pudendal nerve as it transverses through pelvic soft tissue structures such as the piriformis and coccygeus muscles. Cross friction massage, integrative ligamentous releases, and therapeutic ultrasound of the sacrospinous and sacrotuberous ligaments is very effective in alleviating compression at this site. Specific techniques called nerve tissue tension releases and neural mobilization/gliding techniques may improve the mobility and function of the pudendal nerve alleviating symptoms within a few sessions. Malalignment of the pelvis, sacroiliac joints, spine, or coccyx can be a causative or perpetuating factor and are readily addressed by specific manual corrective mobilization or manipulation techniques. Proper bicycle seats, sitting habits and/or postural education will be addressed. Pelvic floor muscle dysfunction rehabilitation with a focus on lengthening, releasing trigger points, relaxing and down-training may be components of your program as this may be another source of your pudendal nerve entrapment symptoms. Prescriptive stretching and strengthening exercises such as hip, lower extremity, and spinal and core stabilization training are instructed. Because of our level of expertise in treating pelvic pain, we have successfully helped hundreds of patients with pudendal nerve entrapment overcome their pain and symptoms.


