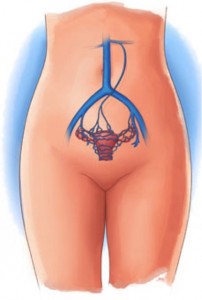
 Pelvic congestion syndrome is a chronic condition that affects women and men and can be a cause of chronic pelvic pain. Typical age effected is between 20 and 45 years old. Patients with pelvic congestion syndrome complain of a severe dull ache or pain in the abdomen, pelvis, groin, and/or genitalia. This can be a result of pelvic varicosities- varicose veins present similar to varicose veins of the legs. Because of vein wall weakness and inability of the vein to return the blood effectively, pressure in the vein increases as blood pools or remains in the pelvic vein. This causes pressure pain, ache, and throbbing which can contribute to nerve irritation in the pelvic region. Vein capacity in varicosities may increase by as much as 60%, especially during pregnancy. Risk factors may include obesity, pregnancy, sedentary lifestyle, constipation, prostatitis, surgeries, ovarian varicosities, and endogenous estrogen levels. Excess estrogen weakens vein walls. The pelvic pain caused by PCS is non-cyclical and lasts more than 6 months in duration. Pain is worsened by sitting, standing, at the end of the day, upon sexual arousal, during or after intercourse. Other symptoms include generalized fatigue, depression, abdominal or pelvic tenderness, lumbosacral neuropathy, rectal pain, and urge to urinate. Female pelvic congestion syndrome is sometimes referred to as ovarian vein reflux and swollen labia, pain prior to menstruation, visible varicosities of the labia, ovarian cysts, and dysmenorrhea (painful periods) are often common issues. Manual exam reveals tenderness upon cervix manipulation, tenderness upon ovary/ uterus/ scrotum palpation, and swelling noted in the surrounding pelvic/groin region. Thickened, tubular veins may be palpated intravaginally or intrarectally. Hemorrhoids, varicose veins of the perineum, buttocks, and lower extremities may also be noted. Pelvic floor muscle dysfunction such as pain, spasm, tender points, trigger points, shortening, and weakness is another common finding. Male pelvic congestion syndrome is underrepresented in medicine and may be mistakenly referred to as prostatitis syndrome. Male pelvic congestion syndrome can be caused by pelvic varicosities and surgery such as varicocelectomy and can be related to varicoceles of the scrotum, prostatitis syndrome, and pelvic floor muscle dysfunction. 50 % of male infertility cases involve pelvic congestion syndrome. Testicular atrophy may also occur. The medical testing includes pelvic ultrasonography (PUS), transvaginal sonography (TVS) with doppler, Magnetic resonance imaging (MRI), computed tomography (CT), and ovarian venography. Medical treatment for pelvic congestion syndrome may consist of hot baths, non-steroidal anti-inflammatory drugs, progestins, phlebotonics, danazol, medroxyprogesterone acetate or gonadotrophin releasing hormone agonist called goserelin, and emolotherapy. For women, surgical ligation of ovarian veins and hysterectomy with or without oophorectomy are also other treatments options. Pelvic physical therapy is a great conservative treatment option.
Pelvic congestion syndrome is a chronic condition that affects women and men and can be a cause of chronic pelvic pain. Typical age effected is between 20 and 45 years old. Patients with pelvic congestion syndrome complain of a severe dull ache or pain in the abdomen, pelvis, groin, and/or genitalia. This can be a result of pelvic varicosities- varicose veins present similar to varicose veins of the legs. Because of vein wall weakness and inability of the vein to return the blood effectively, pressure in the vein increases as blood pools or remains in the pelvic vein. This causes pressure pain, ache, and throbbing which can contribute to nerve irritation in the pelvic region. Vein capacity in varicosities may increase by as much as 60%, especially during pregnancy. Risk factors may include obesity, pregnancy, sedentary lifestyle, constipation, prostatitis, surgeries, ovarian varicosities, and endogenous estrogen levels. Excess estrogen weakens vein walls. The pelvic pain caused by PCS is non-cyclical and lasts more than 6 months in duration. Pain is worsened by sitting, standing, at the end of the day, upon sexual arousal, during or after intercourse. Other symptoms include generalized fatigue, depression, abdominal or pelvic tenderness, lumbosacral neuropathy, rectal pain, and urge to urinate. Female pelvic congestion syndrome is sometimes referred to as ovarian vein reflux and swollen labia, pain prior to menstruation, visible varicosities of the labia, ovarian cysts, and dysmenorrhea (painful periods) are often common issues. Manual exam reveals tenderness upon cervix manipulation, tenderness upon ovary/ uterus/ scrotum palpation, and swelling noted in the surrounding pelvic/groin region. Thickened, tubular veins may be palpated intravaginally or intrarectally. Hemorrhoids, varicose veins of the perineum, buttocks, and lower extremities may also be noted. Pelvic floor muscle dysfunction such as pain, spasm, tender points, trigger points, shortening, and weakness is another common finding. Male pelvic congestion syndrome is underrepresented in medicine and may be mistakenly referred to as prostatitis syndrome. Male pelvic congestion syndrome can be caused by pelvic varicosities and surgery such as varicocelectomy and can be related to varicoceles of the scrotum, prostatitis syndrome, and pelvic floor muscle dysfunction. 50 % of male infertility cases involve pelvic congestion syndrome. Testicular atrophy may also occur. The medical testing includes pelvic ultrasonography (PUS), transvaginal sonography (TVS) with doppler, Magnetic resonance imaging (MRI), computed tomography (CT), and ovarian venography. Medical treatment for pelvic congestion syndrome may consist of hot baths, non-steroidal anti-inflammatory drugs, progestins, phlebotonics, danazol, medroxyprogesterone acetate or gonadotrophin releasing hormone agonist called goserelin, and emolotherapy. For women, surgical ligation of ovarian veins and hysterectomy with or without oophorectomy are also other treatments options. Pelvic physical therapy is a great conservative treatment option.
How can Pamela Morrison Physical Therapy, PC help with Pelvic Congestion Syndrome?
Your expert physical therapist will take a thorough history including medical history and current complaints. Your pelvic floor physical therapist will complete a comprehensive evaluation consisting of an orthopedic assessment of the spine, pelvis, hips, and legs to determine joint mobility, muscle function, alignment, flexibility, neural tension, visceral mobility/motility and neurological function. Posture, movement patterns, and gait pattern are evaluated. The physical therapist will then perform an advanced pelvic floor muscle exam to determine if there is swelling, congestion, compression of pelvic nerves including pudendal nerve involvement, varicosities, or referred pain from other associated orthopedic issues found during the orthopedic exam. Precise systematic palpation of the superficial pelvic floor muscles externally and internally (intravaginally or intrarectally of the deep layer) may reveal tension, pain, trigger points, tender points, spasm, or shortening. Surface EMG (sEMG) biofeedback may be employed to determine if the pelvic floor muscles remain in a constant state of contraction or high-tone. Once your physical therapist determines the orthopedic and pelvic floor muscle exam findings, a treatment plan is individually designed according to the findings. Treatment can consist of advanced manual therapies including joint mobilization, myofascial release, retrograde massage, lymphatic drainage techniques, craniosacral, and integrative manual therapy. Other effective approaches would include therapeutic exercises, pelvic floor muscle rehabilitation including sEMG biofeedback, pain relieving modalities such as electrical stimulation and transcutaneous electrical stimulation (TENS). Sometimes the pelvic floor muscles are weak and performing pelvic floor strengthening exercises such as “kegels” would help support the weakened vein and facilitate drainage of pooled fluid from the pelvic region. Supportive or compressive garments and lymphatic drainage postural positions along with wedges and bolsters are other devices that are recommended. Our patients experience significant symptom relief with our treatments.


